Info-Santé Navig
ROLE
Lead UX Designer
YEARS
2024 - 2025
DURATION
12 months
PROBLEM
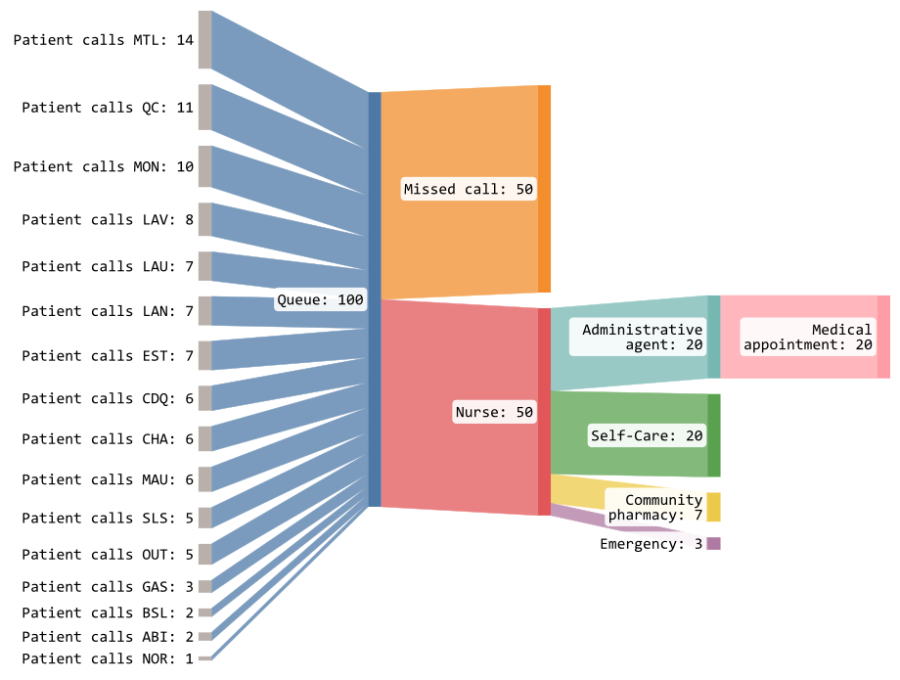
A constrained service causes pressure on the healthcare system instead of reducing it like initially designed
- The Info-Santé 811 service is highly in demand, close to 50% of calls aren’t answered and those that are answered can wait from 30 minutes to 2 hours especially during peak periods.
- This situation is aggravated by the nursing shortage and the current model where nurses answer first.
- This results in a part of the population unnecessarily resorting to the emergency department as a solution which in turn increase the pressure on the healthcare system.
SOLUTION
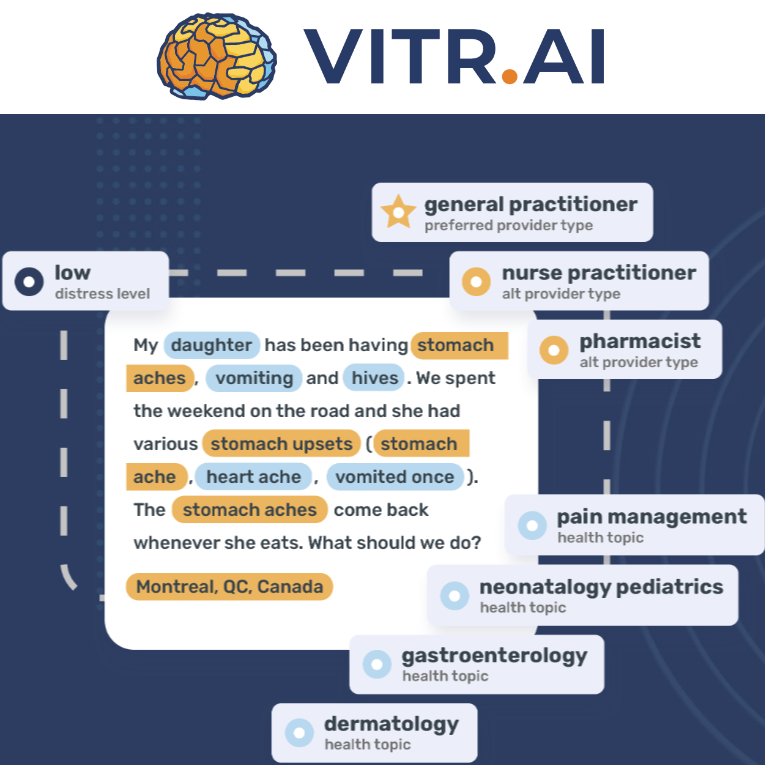
An AI that empowers Info-Santé non-clinical agents to more efficiently route 811 calls
- The solution is to use Vitr.AI’s solution, Navig, an artificial intelligence-based decision support system that assist non-clinical agent to route 811 calls.
- Navig uses patients’ language and clinical rules validated by physicians and nurses to determine the appropriate resource and required timeframe.
- The goal is to route more efficiently calls towards the right care trajectories by empowering administrative agents and ensure that nurses speak to patients that really needs them.
OUTCOME
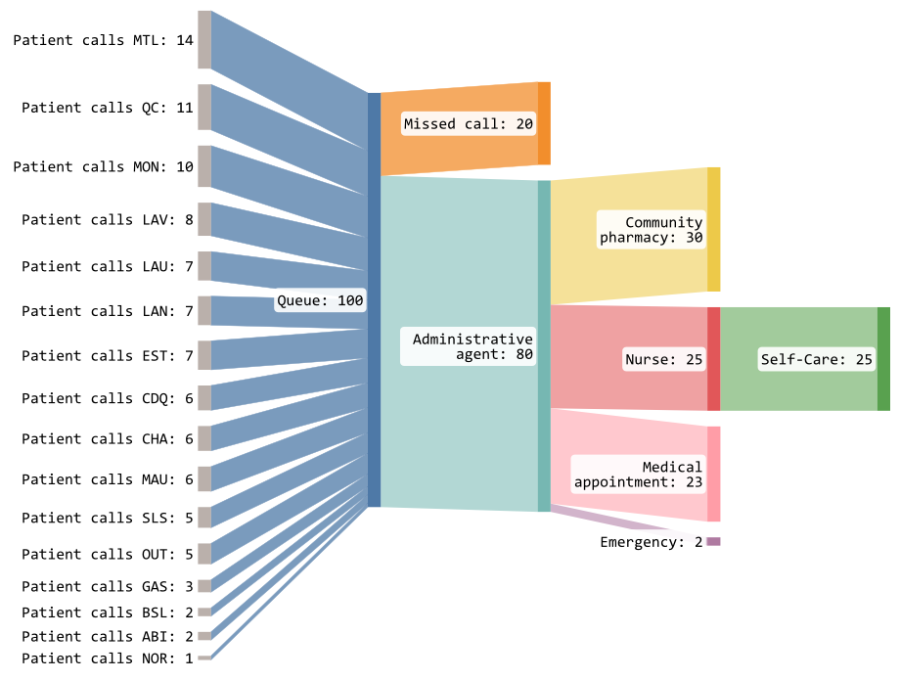
The new workflow’s success has justified its expansion to 811 on a provincial scale.
Wait times were reduced by up to 76%, bringing the average wait time down to 13 minutes.
Call responses improved by 30%, with 80% of incoming calls successfully answered.
1. Discovery
CONTEXT
How do you ensure the success of a solution when the problem isn’t yet properly defined?
- Design is a very new concept in Quebec’s healthcare system, very few people know of this discipline and even fewer acknowledges it.
- This usually put us in unusual situations where the problem is not fully understood but the solution is already chosen.
- We therefore have to find ways to ensure that the solution alleviates the problem as much as possible without going out of scope.
METHODOLOGY
Understanding the pain points of the current workflow
- We need to learn how each stakeholder is feeling about the current workflow and where they would like to see changes.
- A workshop was organized mobilizing patient partners and staff of 811: nurses and administrative agents.
- The purpose of this workshop was to understand the current workflow and offer a space where each participant could share their experiences with the service.

LEARNINGS
Patients voiced their grievances with the current service where almost every step provoked frustration, confusion or distress for them.
Administrative agents expressed the emotional challenges they face when dealing with patients that are at their wit’s end.
Nurses detailed how long it takes to ensure that they are delivering the right care to patients by listing all the tasks they must go through with each patient.

2. Co-creation
METHODOLOGY
Establishing the new care trajectories
- Since only clinicians with a medical license can orient and sort patients, we had to make sure that Navig would offer recommendations based on physicians’ decisions.
- A focus group was conducted with physicians to assess the care trajectories impacted by the project.
- The goal of this focus group was to establish the outcomes of each care trajectory based on a patient’s condition and what would be the physicians’ decisions.

RESULTS
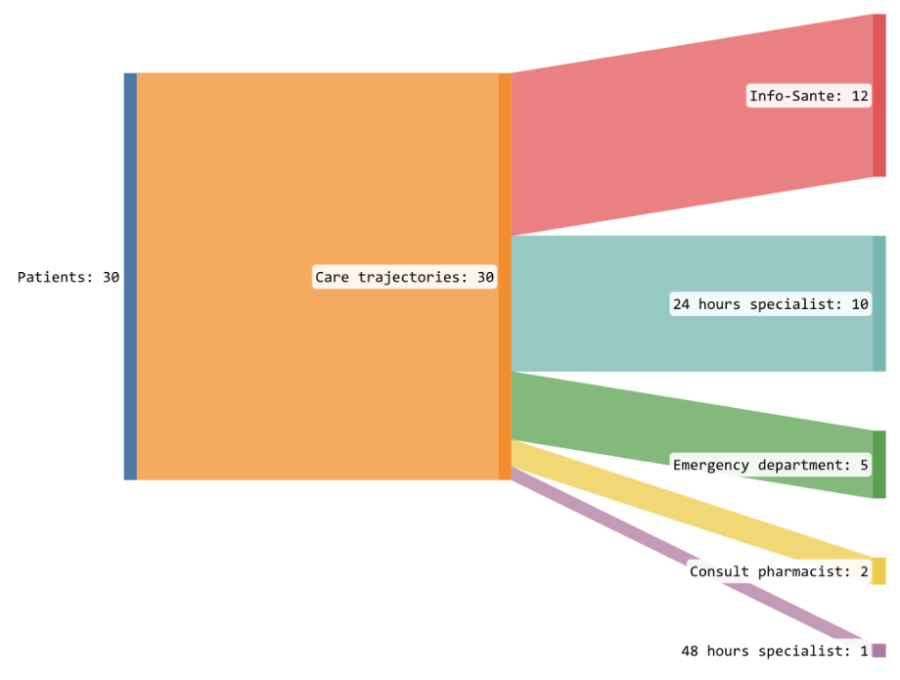
Physicians reviewed a total of 30 care trajectories; each care trajectory would result in one of these orientations:
- Transfer call to Info-Santé
- Schedule an appointment with a specialist within 24 hours and transfer call to Info-Santé
- Send patient to the nearest emergency department
- Send patient to consult a pharmacist
- Schedule an appointment with a specialist within 48 hours and transfer call to Info-Santé
METHODOLOGY
Creating a new workflow that fixes current pain points
- With a better understanding of the service’s pain points and its outcomes, we now have to rethink how the service can be offer to the population.
- A second workshop was planned, this time we mobilize patient partners, nurses, administrative agents, experts in internal processes and managers, the goal was to create a new workflow with Navig.

RESULTS
Participants identify every necessary step the new process would have to take.
They trimmed the process to remove any potential risk of duplication of effort.
Lastly, a list of concerns was brought up to ensure that they would be taken into considerations.

3. Implementation
METHODOLOGY
Refining the new workflow and ensuring all stakeholder concerns are addressed
- The workflow developed through stakeholder collaboration was reviewed with project owners and revised into a standardized process.
- A third and final workshop was convened to present the standardized workflow for stakeholder validation.
- Additionally, stakeholder needs were assessed to identify the materials required for effective onboarding and training, allowing for proper planning ahead of the workflow’s implementation.

RESULTS
Before implementation, the workflow must be refined to ensure clinically safe and nuanced data collection, minimize emotional and operational burden for callers, clarify roles and expectations (particularly at first contact), avoid duplicate assessments, enable seamless information sharing, and transparently manage situations when no appointments are available.
Implementation success is contingent on robust, scenario‑based training, the availability of job aids and live operational support, an iterative pilot process, and a comprehensive communication strategy addressing both internal stakeholders and the general population.
A revised workflow, endorsed by the project owners and validated by all stakeholder groups (patient partners, administrative staff, nursing staff, internal process experts, and managers).
4. Post-mortem
DYNAMICS OF POWER
Understanding and working with political complexity is often the difference between project failure and success
- The workflow developed through stakeholder collaboration was reviewed with project owners and revised into a standardized process.
- A third and final workshop was convened to present the standardized workflow for stakeholder validation.
- Additionally, stakeholder needs were assessed to identify the materials required for effective onboarding and training, allowing for proper planning ahead of the workflow’s implementation.
GROWING PAIN
The systemic failures in healthcare erode trust and can lead to people turning on each other; empathy is crucial when navigating these tense topics
- The healthcare system is showing clear signs of fatigue: clinicians are stretched thin, and the population is waiting longer than ever for care.
- During a workshop, a stakeholder verbalized their dissatisfaction with the healthcare system in a manner that targeted clinicians.
- I stepped in to defuse the situation, which should not have occurred. When addressing sensitive issues, it is critical to cultivate empathy and maintain a respectful dialogue.
SELF REFLECTION
Starting from a place of misalignment and systemic pressure, the project gradually rebuilt trust and shared purpose around improving Info‑Santé 811, with outcomes that speak to the power of collaboration
- The project began under difficult conditions, with unclear alignment among project owners and stakeholders feeling the weight of systemic healthcare challenges.
- By working through these tensions, we were able to reconnect around a shared purpose: improving Info‑Santé This collaboration gradually created empathy and understanding across groups that had previously struggled to work together.
- The results reflect that transformation and stand as a testament to the collective effort behind the project.
Portfolio
Braver Therapy Transfert
How might we design a sustainable approach to therapy transfer that fits real clinical workflows, supports families’ needs, and strengthens continuity of care across settings?

Chroniqueur
How might we present and structure the vast information generated by an emergent narrative simulation so that players can easily uncover, reconstruct, and interpret meaningful stories?